What is Vitiligo?
- Depigmented macules that are the result of melanocytes being damaged and destroyed are the hallmark of the acquired, idiopathic condition known as vitiligo.
- Although the condition can strike at any age, 50% of people develop it before the age of 20.
Description of Vitiligo?
- Long-lasting vitiligo causes the skin to develop pale white patches.
- Lack of melanin, the skin pigment, is causes of it.
- The prevalence of vitiligo is estimated to be around 1% worldwide.
- The skin loses color as a result of the skin condition vitiligo.
- On a person’s skin, smooth white spots (known as macules if less than 5mm in diameter or patches if 5mm or more) can be seen.
- Your body’s hair may turn white if you have vitiligo in an area where you have hair.
- The disorder develops when the body’s immune system kills melanocytes, which are the skin cells that create melanin, the pigment that gives skin its color.
- Despite the fact that vitiligo can affect any part of the body, it most frequently affects the hands, face, neck, and crevasses of the skin.
- Since pale skin is more susceptible to sunburn, additional caution should be used while exposed to the sun and use a sunscreen with best sun protection factor (SPF).
Vitiligo pathogenesis, etiology and causes?
- The typical onset of vitiligo is a few little white patches, which may progressively develop over the body over several months. However, vitiligo can appear anywhere on the body, including the mucous membranes (wet lining of the mouth, nose, genital, and rectal areas), the eyes, and the inner eardrum. It often starts on the hands, forearms, feet, and face.
- The larger patches can occasionally keep growing and spreading, but most of the time they remain in one spot for years. As specific regions of skin lose and gain pigment, the location of smaller macules varies and changes over time. The amount of skin affected by vitiligo varies, with some people having only a few depigmented spots and others having a significant loss of skin colour.
- Where there are hair roots, such as on your scalp, it might also occasionally appear. Your skin’s lack of melanin might cause the affected area’s hair to go white or grey.
- Skin affected by vitiligo frequently begins as a pale area that gradually becomes all-white. A patch’s centre could be white, with paler skin surrounding it. The patch could be somewhat pink rather than white if there are blood vessels under the skin.
- The patch’s margins can be straight or wavy. Sometimes they have a brownish discoloration or are red and irritated (hyperpigmentation).
- Your skin won’t feel uncomfortable from vitiligo, such as dryness, but the patches could occasionally itch.
- Each person has a unique condition, Some people only develop a few little white spots, while others have larger white spots that spread across sizable portions of their skin.
- How much skin will be impacted cannot be predicted. The white spots are typically irreversible.
What are the types of vitiligo?
There are two main types of vitiligo, but some rare types are also discussed below;
- Non-segmental vitiligo (bilateral or generalized vitiligo)
- Segmental vitiligo (unilateral or localized vitiligo)
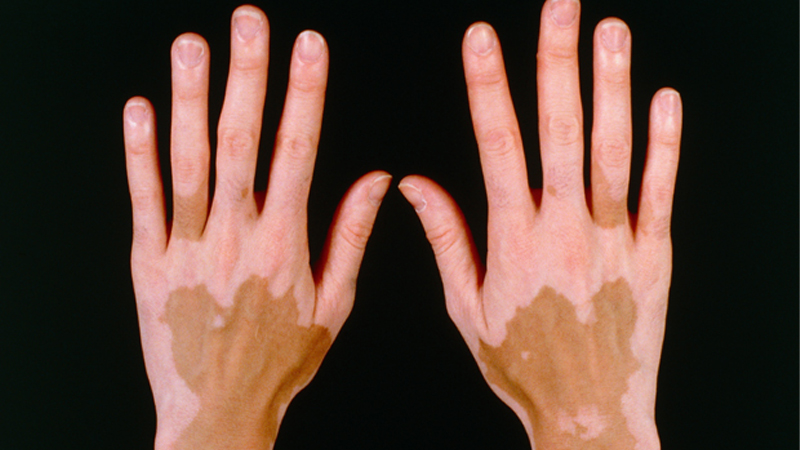
Non-segmental vitiligo (bilateral or generalized vitiligo):
- Non-segmental vitiligo, also known as bilateral or generalized vitiligo, is characterized by symmetrical white patches that frequently develop on both sides of the body.
- The skin around body openings, such as the eyes, the backs of your hands, your arms, your knees, your elbows, and your feet may develop symmetrical patches.
- Around 9 out of 10 patients with vitiligo have non-segmental vitiligo, which is the most prevalent kind.
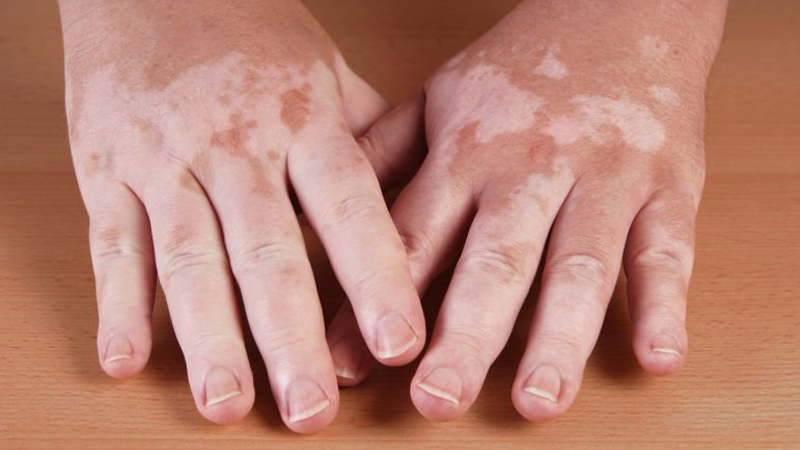
Segmental vitiligo (unilateral or localized vitiligo):
- White patches only appear on one part of your body when you have segmental vitiligo, sometimes referred to as unilateral or localized vitiligo.
- Despite being more common in youngsters, segmental vitiligo is less common than non-segmental vitiligo. In 3 out of 10 children with vitiligo, it typically begins in early age.
Other types of vitiligo also include:
Mucosal:
- It is the type of vitiligo affecting the mucous membranes of the mouth and/or genitalia.
Focal:
- An uncommon variety when the macules are localized in a specific location and do not spread outward over the course of one to two years.
Trichome:
- In which the skin is composed of three distinct regions: a white or colorless center, a region of lighter pigmentation, and a region with the usual color of the skin.
Universal or complete vitiligo:
- Vitiligo can sometimes afflict the entire body, causing more than 80% of the skin on the body to be pigment-free.
- It is referred as universal or complete vitiligo.
Prevalence of vitiligo?
- In the world’s population, vitiligo affects roughly 1% or slightly more of people.
- All races and genders are equally susceptible to vitiligo, however those with darker skin tend to have more obvious symptoms.
- Although vitiligo can arise at any age, it most frequently affects persons between the ages of 10 and 30.
- Very young or very old people hardly ever develop vitiligo.
Causes of vitiligo?
- Lack of melanin, a skin pigment, is the causes of vitiligo. Melanin, which gives your skin its color, is produced by skin cells called melanocytes.
- Lack of functioning melanocytes prevents your skin from producing enough melanin when you have vitiligo.
- Your skin or hair may start to develop white patches as a result.
- The actual cause of the melanocytes’ disappearance from the skin’s afflicted regions is unknown.
There are several distinct theories regarding the causes of vitiligo, despite the fact that they are not all fully established:
Autoimmune Theory:
- The most typical type of vitiligo, non-segmental vitiligo, is assumed to be an autoimmune disease.
- The immune system malfunctions in autoimmune diseases. Your immune system assaults the healthy cells and tissue in your body rather than attacking foreign cells like viruses.
- Your immune system eliminates the skin cells called melanocytes that produce melanin if you have non-segmental vitiligo.
- Although hyperthyroidism (an overactive thyroid gland) and other autoimmune disorders are linked to vitiligo, they are not necessarily developed in all cases of the disease.
Autocytotoxicity Theory:
- According to the Autocytotoxicity theory, keratinocytes or melanocytes themselves can damage melanocytes by releasing substances that cause oxidative stress or by producing melanin precursors (or metabolites) on their own.
- It is thought that vitiligo melanocytes lack the typical defensive mechanisms that protect them from oxidative stress and melanin precursors.
Neurochemicals:
- The less prevalent variety of segmental vitiligo is thought to be brought on by chemicals produced by cutaneous nerve endings.
- The melanocyte skin cells are poisoned by these substances.
Triggers:
Vitiligo may be brought on by specific circumstances, such as:
- skin injury, such as severe sunburn or cuts (this is known as the Koebner response)
- stressful situations, including delivery; (Child birth)
- coming into contact with specific chemicals, such as at work.
- Vitiligo is not an infection, and you cannot get it from someone else who does.
Genetic considerations:
- Some variables that may raise the risk of developing vitiligo can be passed down via families. Vitiligo runs in families in about 30% of instances.
Can vitiligo be inherited?
- Not all cases of vitiligo are inherited. However, roughly 30% of vitiligo sufferers do have at least one close family who also has the condition.
Risk factors for Vitiligo:
You could be more likely to get non-segmental vitiligo if:
- Inherited factor (Family history)
- There is a family history of other autoimmune diseases, such as pernicious anemia in one of your parents (an autoimmune condition that affects the stomach)
- You suffer from another autoimmune disorder.
- You suffer from non-Hodgkin lymphoma (cancer of the lymphatic system) or melanoma types of skin cancer , both of which are type of cancer
- You have specific genetic variations known to be associated with non-segmental vitiligo.
Is vitiligo painful?
- Vitiligo does not cause pain.
- The lighter parts of your skin, however, are more susceptible to painful sunburns.
- It is crucial to safeguard yourself from the sun by taking precautions like applying sunscreen, avoiding the sun during its peak hours, and putting protective clothing.
- Sometimes, even before the depigmentation begins, some vitiligo patients have complained of itchy skin.
Signs and symptoms of vitiligo?
According to dermatologist Suzanne Friedler, MD, who has a private practice in New York City, the formation of light or “depigmented” areas on the skin is the most obvious indication that someone may have vitiligo.
The places with little to no melanin, the skin’s natural pigment, are the areas with the pale patches. These spots may initially occur on exposed skin, such as the face, arms, feet, and hands, but they can appear elsewhere on the body. White spots can also show up around the belly button, in the armpits, and in the groin.
- Premature greying or whitening of the hair is another symptom of vitiligo.
- Withering and turning white eyelashes or eyebrows
- Color loss in the nose and mouth;
- An inflammation of the ears or eyes that causes hearing loss and vision issues;
- Changes in the color of the retina of the eye, according to a study published in the November-December 2019
Different people will experience skin spots in different places and at different rates of spread and progression.
Problems associated with vitiligo?
Even though vitiligo is mostly a cosmetic disorder, those who have it may face a number of issues:
- Rather than tanning, macules will burn because they lack melanocytes, making them more susceptible to sunlight than the rest of the skin.
- The inner layer of the eye that includes light-sensitive cells, the retina, may exhibit some abnormalities in vitiligo patients, as well as some fluctuation in iris color (the colored part of the eye).
- Although the retina or iris may occasionally become inflamed, vision is typically unaffected. Vitiligo patients may have an increased risk of developing other autoimmune disorders, such as hypothyroidism, diabetes, pernicious anemia, Addison’s disease, and alopecia areata, in which the body attacks itself.
- Additionally, vitiligo is more likely to affect those who have autoimmune illnesses.
- Vitiligo patients could experience anxiety or embarrassment over their skin. People might be nasty at times; they might glare or say hurtful things.
- A person with vitiligo could become self-conscious as a result of this. As a result, someone may experience anxiety or sadness and feel the need to withdraw. If this occurs, you should consult your doctor or your family and friends to assist you come up with a plan of action.
Complications of vitiligo:
- Other issues might occasionally result from vitiligo.
- Your skin will be more sensitive to the impacts of the sun since you lack melanin.
- To prevent sunburn, use a high-quality sunscreen.
- Inflammation of the iris, inflammation of the central layer of the eye (uveitis), and a partial loss of hearing (hypoacusis) are all possible side effects of vitiligo.
- People with vitiligo frequently experience issues with confidence and self-esteem, especially if the condition affects exposed skin parts.
Diagnosis of vitiligo?
Usually the white patches are easily visible on the skin, a healthcare provider will be able to diagnose vitiligo after examining the affected areas of skin.
This may include;
- They might inquire about your family history of vitiligo
- Other autoimmune diseases
- Injuries to the affected areas of skin (such as sunburns or severe rashes)
- How easily you tan or burn in the sun
- Whether any areas of your skin have improved or gotten worse without treatment, and whether you’ve tried any treatments previously.
A medical practitioner may also bring up the impacts of vitiligo on your life. For example, how much it affects your self-esteem and confidence, and whether it affects your career.
Wood’s lamp:
- If one is available, the medical professional might use a Wood’s light to examine your skin more closely.
- The lamp must be held 10 to 13 cm away from your skin, and you must be in a completely dark environment.
- Under UV light, the vitiligo patches will be more visible, allowing medical professionals to differentiate vitiligo from other skin disorders like pityriasis versicolor (when there is a loss of pigment due to a fungal infection).
Diagnosis of autoimmune conditions:
You may be examined to check if you have any symptoms that could imply an autoimmune disorder because non-segmental vitiligo is closely linked to other autoimmune conditions, such as:
- feeling tired and depleted in energy, which could indicate Addison’s disease
- experiencing frequent urination and thirst, which could be symptoms of diabetes
Blood test:
- You might also require a blood test to see how effectively your thyroid gland is functioning.
Other conditions resembling to vitiligo?
Other disorders can alter or cause the skin to lose pigment.
These consist of:
Chemical leukoderma:
- Linear or splotchy white patches of skin appear after exposure to certain industrial chemicals damages skin cells.
Tinea versicolor:
- This yeast infection can produce light or dark patches that are visible on different skin tones.
Albinism:
- This genetic condition results in a person’s skin, hair, and/or eyes having fewer levels of melanin than normal.
Pityriasis alba:
- This condition causes red, scaly patches of skin that eventually turn into lighter, scaly patches of skin.
Treatment of vitiligo?
- Consider therapy if your vitiligo is severe or if it is causing you any discomfort.
- Vitiligo does not have a treatment.
- Medical treatment aims to achieve a uniform skin tone by either repigmenting (restoring color) or removing the remaining color (depigmentation).
- Surgery, light therapy, repigmentation therapy, and camouflage therapy are all common forms of treatment.
- Additionally, counselling might be advised.
Medication for Vitiligo;
In some cases, medicines can reduce the severity of vitiligo, these medications may include;
Corticosteroid creams are one form of treatment.
- Topical medications with tacrolimus or pimecrolimus,
- Topical vitamin D substitutes (which are synthetic versions of the vitamin)
- Combination therapy with UVA light and the oral medicine psoralen, which may be especially successful if you have significant regions of skin affected by vitiligo.
- Combination therapy with UVA light and the oral medicine psoralen, which may be especially successful if you have significant regions of skin affected by vitiligo.
- Methoxsalen and other repigmentation agents;
- Monobenzone cream for the removal of pigment from unaffected skin
- A novel treatment for vitiligo is tacrolimus, a macrolide immunosuppressant derived from the fungus Streptomyces tsukubaensis.
- The US Food and Drug Administration has approved topical tacrolimus for the treatment of atopic dermatitis. It has been approved for use in children 2 to 15 years old at a concentration of 0.03 percent, and in adults at a concentration of 0.1 percent.
- Tacrolimus has also been used successfully and safely to treat skin conditions with an immunological basis, such as psoriasis, pyoderma gangrenosum, and alopecia areata.
Camouflage therapy:
- Using sunscreen with an SPF of at least 30. Additionally, sunscreen must block both ultraviolet B and ultraviolet A light (UVB and UVA). Sunscreen use reduces tanning, which reduces the contrast between damaged and normal skin.
- Makeup can conceal regions that lack pigment. The Dermablend® brand is one popular one.
- If vitiligo affects the hair, hair colors may be utilized.
- If the illness is severe, depigmentation therapy with the medication monobenzone may be used. When applied to pigmented skin patches, this medicine will make them white so they resemble vitiligo-affected areas.
Repigmentation therapy:
- Corticosteroids can be used topically (as a cream put on the skin) or taken orally (as a tablet). Results could take three months.
- If the medication is used for an extended time period, the patient may experience some side effects like striae (stretch marks) or skin thinning, which the doctor will check for.
Repigmentation therapy includes;
- Topical analogues of vitamin D.
- Topical immunomodulators, such as inhibitors of calcineurin.
Light therapy:
- For several months, two to three treatment sessions per week are needed for narrow band ultraviolet B (NB-UVB).
- Excimer lasers produce ultraviolet light with wavelengths that are comparable to narrow band UVB.
- Since it is administered to small, precise regions, it is helpful for people who do not have extensive or huge tumors.
- To treat extensive vitiligo skin lesions, oral psoralen and UVA are combined (PUVA).
- The head, neck, torso, upper arms, and legs of those who have vitiligo are believed to respond quite well to this therapy.
Surgery:
Autologous skin grafts (from the patient):
- Skin is removed from one portion of the patient and applied to another. Scarring, infection, or a failure to repigment are examples of potential side effects.
- Another name for this is mini-grafting.
Micropigmentation:
- A form of tattooing typically done on the lips of vitiligo sufferers.
Counseling:
- Psychological discomfort brought on by vitiligo might influence a person’s worldview and social interactions.
- In this situation, your caregiver might advise you to locate a counsellor or join a support group.
How can I prevent vitiligo?
- Nobody can advise you on how to avoid vitiligo because no one is certain of what causes it.
- It is generally a good idea for everyone to take proper care of their skin and adopt safe sun exposure practices.
Outlook for people with vitiligo?
- About 10 to 20 percent of vitiligo patients completely regain their skin color.
- Young people with vitiligo that mostly affects the face and reaches its peak in less than six months have the best chances of restoring skin color.
- People who get vitiligo on their lips and limbs, particularly the hands, later in life have a lower chance of regaining their color.
Is vitiligo fatal?
- No. Additionally, it is not at all communicable.
What should I know about living with vitiligo?
- You may come across the idea that “vitiligo is not life-threatening, but it is life-altering” when reading about the condition.
- One explanation for this is that vitiligo evolves through time.
- Another aspect is that being unusual should be avoided in many communities, which place a high value on appearance. For women, this is frequently quite true.
- Everyone needs to take responsibility for their health.
- The goal is to get knowledgeable about vitiligo and find a doctor who is knowledgeable about the condition and available treatments.
- Make sure to communicate with your medical provider if any new symptoms emerge that worry you or if you have inquiries.

